Am I seeing more of this in clinic than ever before? I’m not sure. Maybe. But it’s certainly a pest for those struck down and the tendency for it to be mislabelled is a big problem as conventional acne treatment based on an antibiotic regime will make matters worse.
What is Fungal Acne?
So the problem lies in the humble follicle. We’re all colonised with the yeast-y fungus Malassezia furfur after our sex hormones switch on our oil glands at puberty. Malassezia was previously known as Pityrosporum ovale, but it got a groovy new name - however they’re the same organism. It usually sits quietly, occupying its place in the skin’s microbiome, not causing much bother. But in certain instances - humid conditions, under the influence of oily unguents, after a course of antibiotics - it grows bold and starts to flourish, and can start to trigger inflammation. In some, the presence of this organism on the skin will cause seborrhoeic dermatitis - a red, scaly rash of the eyebrows, nasal creases and scalp. For others, it causes inflammation of the hair follicle - folliculitis - and voila, you’ve got what is now commonly referred to as fungal acne.
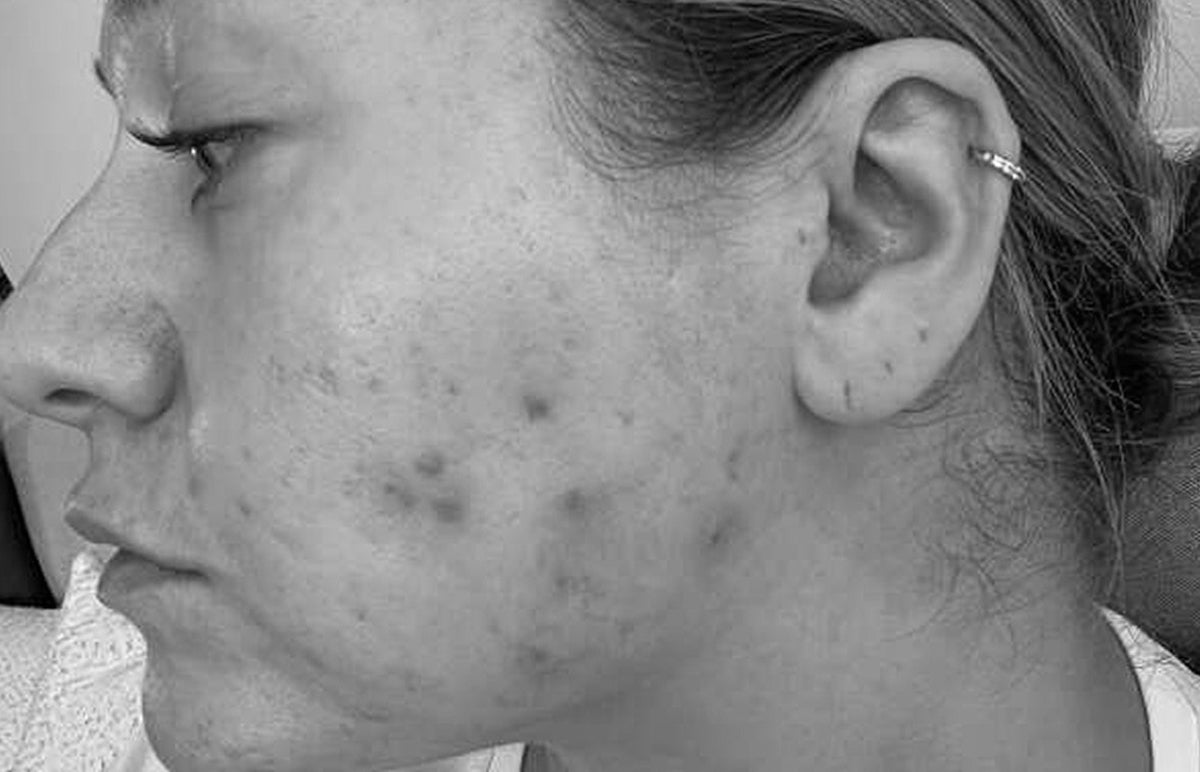
So when someone comes to see me in clinic with this sort of an issue, there’s a fairly classical appearance to the skin. We see fine red bumps with little white heads (pustules) and there are lots of them - and they all look the same. This is quite often different to acne vulgaris, where you see comedones (blocked pores) and varying inflamed lesions, which might be little (papules and pustules) or big (nodules and cysts). The distribution is also different - foreheads and temples are often affected, whereas in adult women, acne vulgaris typically strikes the lower face, the U-zone. I’ll often note the presence of dandruff in the scalp - seborrhoeic dermatitis may well be present coincidentally.
How To Treat Fungal Acne
Now of course, life being a tricky bugger, it’s possible to have both fungal acne and acne-acne at the same time. Oily sebaceous glands are the centre of the action in both. But best to treat the fungal bit first and then see what you’re left with.
I tend to find that the group that present to me warrant oral antifungals, such as fluconazole. Patients need to be warned about tummy upset and the possibility of liver inflammation. Response tends to be prompt - which is good news. Recurrence is frequent. Which is less so.
But you can encourage remission with the use of a topical antifungal shampoo, like Ketoconazole. So try mixing it in with a gentle cleanser to make it easier. Other ingredients that can help include zinc pyrithione and selenium sulphide. However I find ketoconazole more effective in general.
Once that’s all going nicely, I’ll treat any residual acne with topical retinoids, benzoyl peroxide, and azelaic acid (staying away from all antibiotic-containing topicals). And do a bit of a skincare detox to simplify their routine and eliminate any facial oils. A final note - this same approach works well for the body too; be sure to shower promptly after exercise, especially sweaty activities like HIIT and spinning.