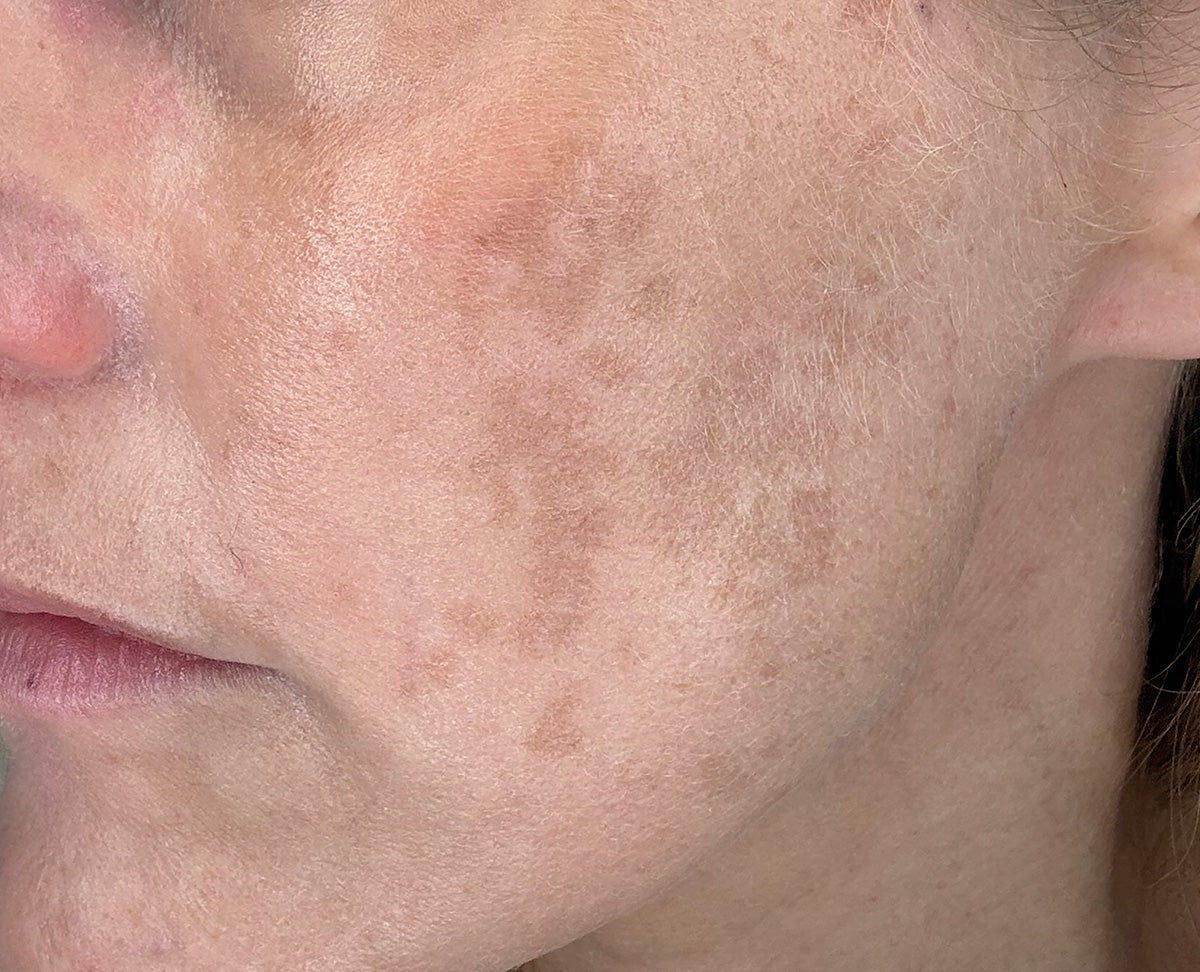
Have you ever met anyone who is happy with their pigmentation? It’s certainly become the aspect of ageing that my patients are keenest to address. And I think that’s because we’re hardwired to like looking at bright, even-toned skin it screams ‘healthy’. But what’s really at the root of the issue?
Pigmentation in skin is usually due to excess melanin, the pigment that protects skin from UV exposure. There are numerous causes – the commonest being issues like sunspots (medically, known as solar lentigos), melasma and post-inflammatory pigmentation (for instance, after acne blemishes). And darker skin-types are inherently more at risk of issues of pigmentation, than fairer skin tones.
I thought it might be helpful to create a practical guide to the major problems I see in the clinic when it comes to managing my patients with a tendency to pigmentation. Whilst there are differences, depending on the cause, there are definitely some common red flags!
1) Don’t skimp on UV protection
Pigmentation often affects those who tan easily, so it can be easily dismissed as not being important skincare fundamental. However, in all instances, UV exposure will tend to exacerbate your pigmentation so the first step is to build proper broad-spectrum sunscreen into your day-to-day skincare routine and limit exposure by avoiding sun exposure between 11 am – 3 pm and covering up. I prefer mineral-based sunscreen in those with hyperpigmentation as I feel it offers the best protection against the deeply penetrating UVA rays we are exposed to all year round which can also travel through glass. Get into the habit of measuring your SPF out properly, not skipping a bit (the hairline is so often not fully protected) and reapplying it if in direct sunlight.
2) Avoid picking, scratching or squeezing – this one’s obvious but needs reinforcing. Any intervention with an inflamed blemish carries risk – of driving inflammation deeper into skin (in which case it might scar) and of triggering more irritation, which drives the pigmentation to get darker. You know my advice – treat it (BPO or salicylic acid), cover it (Dermablend), distract (winged eyeliner at the ready).
3) Don’t do hair removal without thinking it through – waxing, especially with hot wax can be problematic on pigmentation-prone skin, particularly if then combined with UV exposure. So don’t get caught out at the beauty parlour!
4) Don’t skimp on SPF post-procedure.
Following on from my last point, remember that treated skin is usually vulnerable, whether you’ve had peels, laser or microdermabrasion. Take a hat that properly protects your face (7cm brim, UPF rating) and discuss safe use of SPF with whomever has done your treatment.
5) Don’t skimp on metal.
Remember visible light can trigger pigmentation – so look for products with iron oxide to neutralise the double whammy of UV and visible light. And remember your daytime antioxidant serum to mop up free radicals.
6) Think carefully about hormonal contraception – especially in summer. One of the commonest triggers for melasma is UV exposure after starting the combined Pill. Of course, everything in medicine is a balance of risk and benefit, but I do find that for some of my patients, the risk wasn’t something they properly considered.
7) Don’t source pigmentation products from unverified sources. There’s a real problem with black market skin bleaching agents, many of which won’t contain a list of the ingredients they contain. High potency steroids and excessively high concentrations of hydroquinone have been reported and can lead to appalling side effects. This class of skin creams should only be used on prescription under dermatologist guidance, as these products cannot be used indefinitely.
I hope that these tips help you feel more confident in how you approach your pigmentation – remember, a consistent and considered approach to your skincare routine is the secret to success. Wishing you Good Skin Days!
Dr Sam